Supraclavicular lymph node swollen2/19/2024 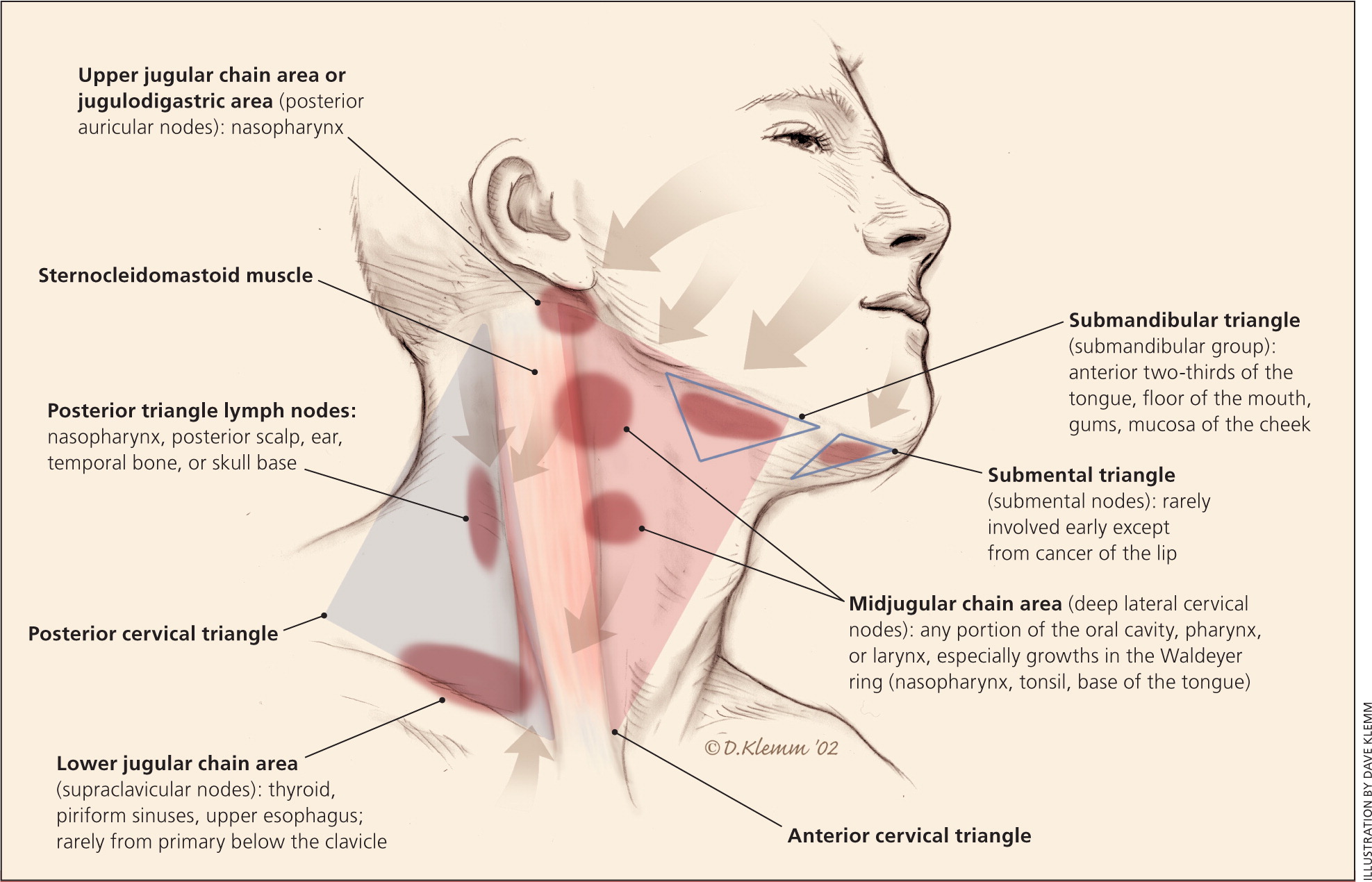 
This patient underwent bilateral orchiectomy and adjuvant hormonal therapy and survived for 47 months after diagnosis of left supraclavicular node metastasis. Prostate-specific antigen levels and magnetic resonance imaging findings aided the diagnostic process. In the prostate carcinoma case, 18F‐fluorodeoxyglucose uptake was weak. He survived for 2 months after diagnosis of left supraclavicular lymph node metastasis. GATA3 staining aided in the diagnosis of urothelial bladder cancer with left supraclavicular node metastasis. Hematoxylin–eosin staining of the bladder lesion did not identify a clear glandular or squamous component, and we could not make a definitive diagnosis of whether the lesion was poorly differentiated squamous cell carcinoma, adenocarcinoma, or high-grade urothelial carcinoma. In the bladder carcinoma case, pathological analysis of fine-needle aspiration biopsy specimen of the metastatic cervical lymph node showed atypical cells with slight squamous differentiation. Palliative care only was given, with survival for 11 months after diagnosis of lymph node metastasis. In the cholangiocarcinoma case, carbohydrate antigen 19-9 and alpha-fetoprotein levels helped to diagnose cholangiocarcinoma. In these cases, adenocarcinoma was diagnosed based on left supraclavicular node biopsies, and a second primary tumor was found, in a 78-year-old Japanese woman with a diagnosis of cholangiocarcinoma, a 64-year-old Japanese man with a diagnosis of bladder carcinoma, and a 61-year-old Japanese man with a diagnosis of prostate carcinoma. We report three cases of malignant infradiaphragmatic tumor diagnosed following an initial finding of left supraclavicular node metastasis after surgery for tongue squamous cell carcinoma (follow-up period, range 18–62 months). When metastasis is detected in the left supraclavicular node in patients with head and neck carcinoma, locating the primary cancer remains a difficult and time-consuming challenge despite the dramatic development of screening technologies and treatment methods. "But the size is not really an issue, as much as how the patient is coping with it.Metastasis of infradiaphragmatic tumors to the left supraclavicular lymph node is reported to be rare. "If you're really worried, you can seek treatment," Dr Price said. While engorged lymph nodes may look pretty confronting - not to mention uncomfortable - they do tend to start subsiding in a week or so, says Karen Price, president of the Royal Australian College of General Practitioners. While Mr Nevill's lymph nodes didn't swell up, people have reported lumps appearing in their armpit - some as big as an orange. "Our immune system has a spectacular number of different subsets, and they all work together," Dr Groom said. Some people might also get relatively large amounts of spike protein ferried to their lymph nodes quickly, contributing an extra burst of inflammation.īut if you don't get lymph node swelling or any other commonly reported effects such as lethargy and fever after your COVID booster, that doesn't mean you've not generated a strong immune response.Ī fifth to a quarter of people who received two doses of the Pfizer vaccine reported an adverse event of some kind, but vaccine efficacy was around 95 per cent. When a COVID vaccine is injected into your arm muscle, your body starts building SARS-CoV-2 virus spike proteins. They help your body fight off infections, but also play a vital role in generating immunity via vaccines. Lymph nodes or lymph glands are (usually) small bean-shaped lumps of tissue found throughout your body and connected in a network by lymph vessels. So why might your lymph nodes arc up after a COVID booster, and when should you see a doctor about it? What are lymph nodes, anyway? 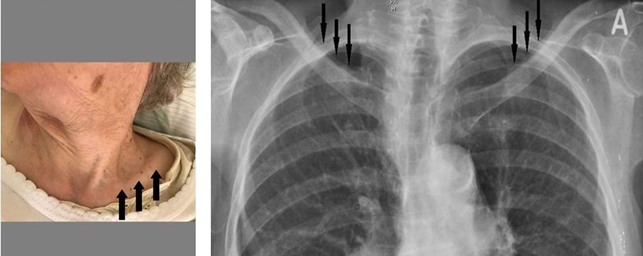
That's in contrast to less than one in 100 after their first or second shot. Read our full coverage of the coronavirus pandemicĪccording to the first Therapeutic Goods Administration's COVID vaccine safety report of 2022, swollen lymph nodes (also called lymphadenopathy) was the most commonly reported "adverse event" or unintended effect following a booster or third dose.Ĭlinical trials show up to one in 20 (Pfizer) and one in 10 people (Moderna) will get swollen or sore lymph nodes following a booster. "It was like someone grabbed my t-shirt on the back of my shoulder and yanked it tight under my armpit."ĭespite getting mRNA vaccines for his first two doses, this was the first time he'd experienced painful lymph nodes.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
